Ulcerative colitis is a chronic inflammatory bowel disease that affects the colon and rectum. Managing this condition requires a multidimensional approach, with diet playing a significant role in symptom management and overall well-being. In this article, we will explore the relationship between diet and ulcerative colitis, providing insights into dietary strategies, food choices, and lifestyle modifications that can help individuals with this condition lead a healthier and more comfortable life.
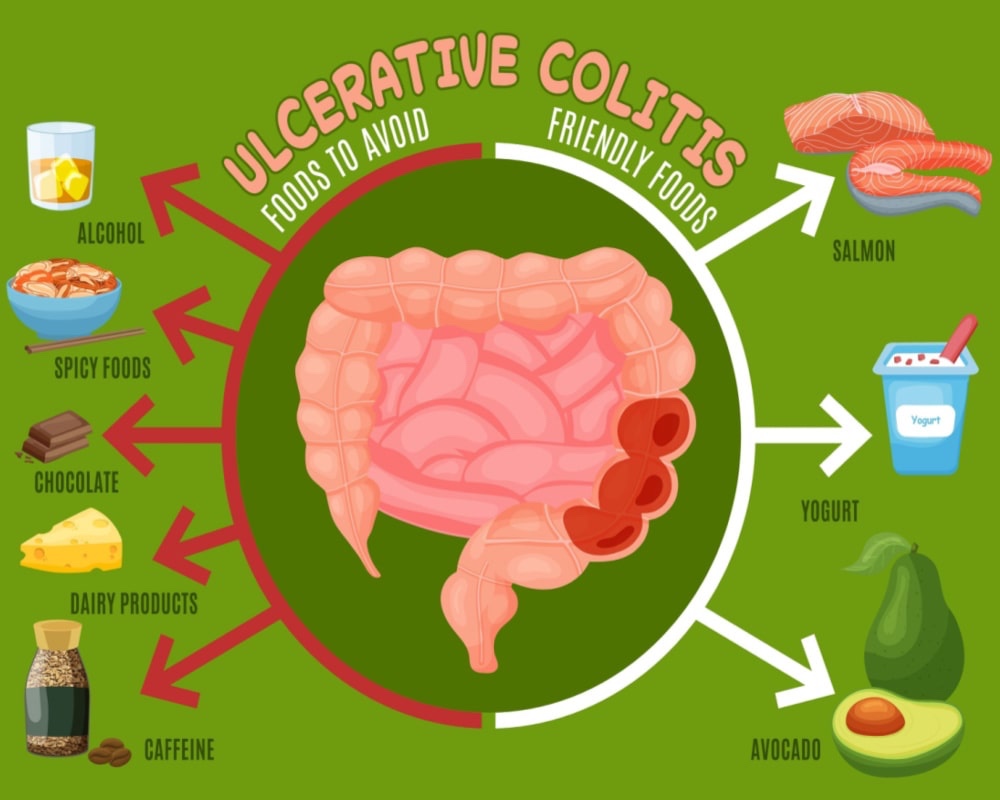
Understanding Ulcerative Colitis: Ulcerative colitis is characterized by inflammation and ulceration of the inner lining of the colon and rectum. While diet alone cannot cure ulcerative colitis, certain dietary modifications can play a vital role in managing symptoms and reducing inflammation.
Dietary Strategies for Ulcerative Colitis:
- Low-Residue Diet: During flare-ups or periods of active inflammation, a low-residue diet may be recommended. This diet focuses on consuming easily digestible, low-fiber foods to minimize bowel irritation and promote healing.
- Specific Carbohydrate Diet (SCD): The SCD is a restrictive diet that eliminates complex carbohydrates, grains, and processed foods. It emphasizes nutrient-dense, easily digestible foods to alleviate inflammation and support gut health.
- Anti-Inflammatory Foods: Incorporating anti-inflammatory foods such as fatty fish, leafy greens, turmeric, ginger, and olive oil can help reduce inflammation in the gut and promote healing.
- Fiber Management: While high-fiber foods are generally considered beneficial for digestion, individuals with ulcerative colitis may need to monitor their fiber intake. Gradually increasing fiber and incorporating soluble fiber sources like oats, apples, and bananas can be helpful in maintaining bowel regularity.
- Hydration: Staying hydrated is crucial for individuals with ulcerative colitis. Drinking an adequate amount of water throughout the day can prevent dehydration and support overall digestive health.
- Food Diary and Personalization: Keeping a food diary can help identify trigger foods and individual sensitivities. Working with a registered dietitian or healthcare professional can further personalize dietary recommendations based on individual needs and preferences.
Lifestyle Modifications for Ulcerative Colitis: In addition to dietary changes, certain lifestyle modifications can contribute to the management of ulcerative colitis. These may include stress management techniques, regular exercise, and adequate sleep. Engaging in relaxation practices such as meditation, yoga, or deep breathing exercises can help reduce stress and promote overall well-being.
Diet plays a significant role in managing ulcerative colitis and alleviating its symptoms. While there is no one-size-fits-all approach, adopting a personalized dietary strategy, including low-residue or specific carbohydrate diets, incorporating anti-inflammatory foods, managing fiber intake, and staying hydrated can contribute to symptom relief and improved quality of life. It is important to work closely with healthcare professionals, such as gastroenterologists and registered dietitians, to develop an individualized plan that suits your specific needs and helps you navigate the challenges of living with ulcerative colitis. By taking a holistic approach that combines proper nutrition, lifestyle modifications, and ongoing medical care, individuals with ulcerative colitis can optimize their well-being and find relief from symptoms.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.




